Healthcare Design Considerations in the Wake of COVID-19
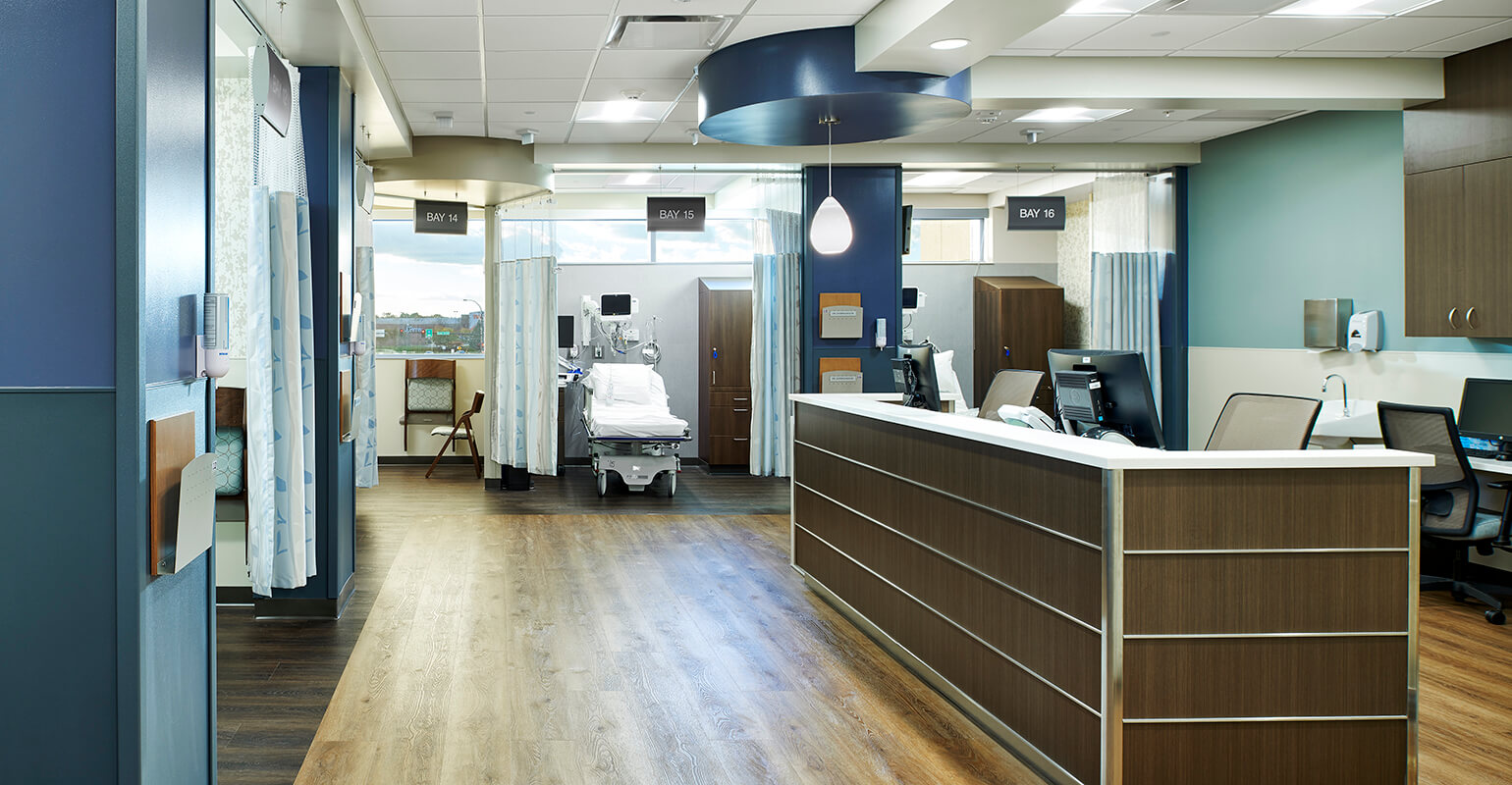
The novel coronavirus has dynamically upended our daily lives and instigated a substantial shift in what we once considered normal. In a time of unprecedented change, we know that healthcare facilities need to be reimagined to withstand the current pandemic and prepare us with progressive environments for the future. We now think very differently about how we respond to change on so many levels. We have used the lessons we learned during the response to the coronavirus pandemic to identify six key design considerations to maximize the patient experience and improve efficiencies among staff in the wake of COVID-19.
Contingency Planning
![]()
As experts in creating transformative design for healing, we understand that scenario planning is vitally important to designing effective and forward-thinking healthcare facilities that support changed behaviors, new safety protocols, and provide continuity of care. Assessing space needs and various scenario planning during the programming phase of design will result in resilient healthcare environments capable of prevailing during challenging times by remaining operable, agile and safe.
Flexibility
COVID-19 taught us that curve balls come when we least expect them and in order to overcome unexpected challenges, clinic spaces need to be easily adaptable. Flexibility will be paramount for clinics of the future, requiring medical spaces to serve multiple functions while also considering the resources of the healthcare practice. The design of a robust mechanical system should be considered. Preparedness scenario planning may present the need for outpatient clinics to provide rooms with negative air pressure to protect staff and patients and reduce the risk of infection. Incorporating elevated technology and MEP infrastructure will enable outpatient environments to be easily converted to meet patient surge capacities.
Innovative Technology

Telehealth services rapidly expanded during the pandemic. The onset of COVID-19 elevated both the need for, and comfort level associated with using virtual care. The lighting, acoustics, backdrop and placement of equipment in exam rooms will need to be thoughtfully designed to cultivate a quality virtual care experience, and a secure platform will be essential to providing a safe care environment and maintaining patient privacy. There will be opportunities to evaluate the effectiveness of virtual care and square footage requirements associated with offering telehealth services.
Process Innovation

Now is the time to challenge and reimagine processes to improve patient care. The patient check-in process should be evaluated for improved efficiencies. Staggering patient appointment times can reduce waiting area capacity, and self-check-in and self-rooming have the potential to decrease wait times and limit reception staff’s exposure to infectious disease. If physical distancing is preferred, then increasing the square footage of the waiting area should be considered. During heightened levels of risk, consider drive-thru testing or vaccine distribution to reduce the risk of cross-contamination and undue exposure. Advancements in technology will support the expanded telehealth services and improved monitoring devices will allow for better patient self-care management.
Material Selection
![]()
It is crucial to identify high-touch surfaces and install materials that are conducive to CDC recommended cleaners and that can withstand the increased cleaning protocols required to mitigate the risk of infection. In addition to finish selections, furniture will also need to withstand the same increased cleaning protocols. When making material selections, life cycle costs, maintenance requirements, acoustical performance, comfort and visual aesthetics will be key elements of evaluation.
Touchless Technologies

Incorporation of touchless technologies should be considered to diminish the need to touch surfaces. Touchless technologies can include motion sensor lighting controls, automatic door operators, motion sensor faucets and flush valves. It will be imperative to provide access to either automatic hand sanitizer dispensers or hand-wash stations in high-traffic areas such as lobby spaces, building entrances and care team areas. Increased access will encourage patients and staff to wash their hands more frequently.
BDH is committed to supporting healthcare practices and systems, facility managers and developers as we navigate through this rapidly changing landscape. Contact us to start transforming your medical property into a flexible, adaptable and resilient environment today.
